Metabolic encephalopathy is a condition where brain function is impaired due to metabolic imbalances in the body. Common causes include nutrient deficiencies, organ failures, and systemic illnesses. Recognizing symptoms like confusion, agitation, and memory loss early can lead to effective treatment. This article delves into the causes, symptoms, diagnosis, and treatment options for this complex condition.
Key Takeaways
- Metabolic encephalopathy is caused by underlying metabolic issues, presenting diverse cognitive and physical symptoms that can escalate to life-threatening conditions if untreated.
- Early diagnosis and comprehensive treatment, including addressing root causes and managing acute metabolic derangements, are essential for improving patient outcomes and preventing complications.
- Critically ill patients are at higher risk for drug-induced metabolic encephalopathy, necessitating vigilant monitoring and a multidisciplinary approach to effectively manage their condition.
Defining Metabolic Encephalopathy
Metabolic encephalopathy refers to a brain dysfunction caused by an underlying metabolic issue, which can range from nutrient deficiencies, including thiamine deficiency and vitamin deficiencies, to organ dysfunction. This condition manifests in various forms, including acute metabolic encephalopathy, toxic metabolic encephalopathy, and wernicke encephalopathy. Acute cases often result from deficiencies in essential nutrients like vitamins, glucose, or oxygen, while toxic cases arise from organ failures that lead to the accumulation of toxic elements in the body.
The symptoms of metabolic encephalopathy are diverse and can appear suddenly or develop gradually over time. Common cognitive symptoms include confusion, disorientation, and memory problems. Patients may also experience hallucinations, agitation, and noticeable personality changes, such as increased irritability. Physical symptoms can include involuntary movements like tremors and seizures, making the condition even more challenging to manage.
Recognizing different types of metabolic encephalopathies aids in accurate diagnosis and appropriate treatment. Conditions like hepatic encephalopathy, uremic encephalopathy, and hypoxic-ischemic encephalopathy each have unique underlying causes and require specific interventions. Recognizing the varied symptoms and their potential severity helps in identifying the condition early and improving patient outcomes.
Common Symptoms of Metabolic Encephalopathy
The symptoms of metabolic encephalopathy can significantly impact how your brain functions, leading to a range of cognitive impairments, including pre existing cognitive impairment. Patients often experience confusion, disorientation, and memory problems, which can severely disrupt daily life. This cognitive impairment, often referred to as mild cognitive impairment in its early stages, can progress to more severe forms of global cerebral dysfunction if not addressed promptly.
Physical symptoms are also prevalent in metabolic encephalopathies. These can include nausea, fatigue, and difficulty sleeping, which often leads to insomnia. Such symptoms not only affect the patient’s physical well-being but also compound the cognitive issues, creating a vicious cycle that can be hard to break without proper physical exam medical condition intervention.
In severe cases, the symptoms of metabolic encephalopathy can escalate to impaired consciousness, loss of consciousness, or even coma. This highlights the critical need for early recognition and treatment of the condition to prevent these life-threatening outcomes. Understanding the full spectrum of symptoms, from mild cognitive impairment to severe brain dysfunction, is essential for timely and effective treatment.
Underlying Causes and Risk Factors
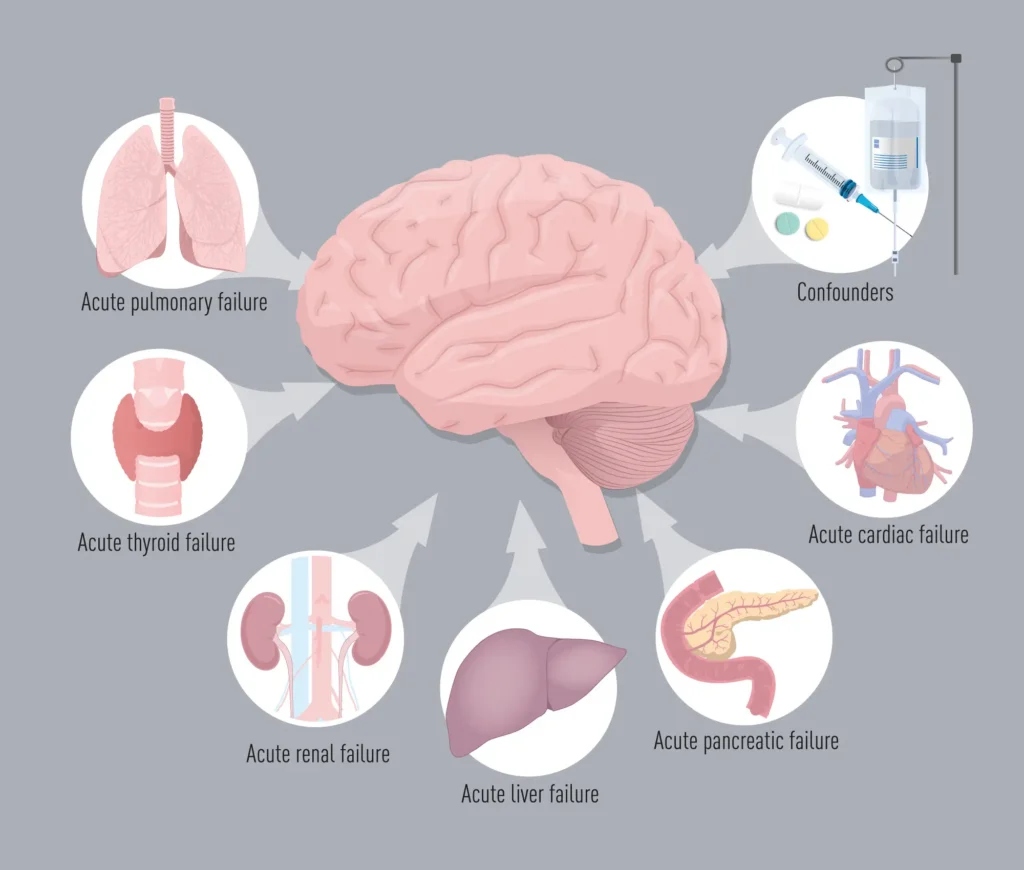
The underlying etiology of metabolic encephalopathy often involves systemic diseases and health problems that disrupt the body’s metabolic processes. Liver failure is a common underlying cause of liver disease, as it impairs the body’s ability to detoxify harmful substances, leading to toxic metabolic encephalopathy. Similarly, renal failure can cause an accumulation of waste products in the blood, triggering encephalopathy, organ failure, and hepatic failure can further complicate these conditions.
Metabolic disorders such as malnutrition and pancreatitis can also lead to metabolic encephalopathy may by disrupting essential metabolic functions. These conditions highlight the importance of maintaining overall health to prevent complications. Hospital-acquired infections, as illustrated by a case study of a 52-year-old woman who developed encephalopathy during hospitalization for sepsis, also pose significant risks.
Identifying the risk factors associated with metabolic encephalopathy is vital for prevention and early intervention. Systemic illnesses, organ failures, and metabolic disorders all contribute to the development of this condition. Identifying and managing these underlying health risks can help prevent the onset of metabolic encephalopathy and improve patient outcomes.
Diagnosing Metabolic Encephalopathy
Diagnosing metabolic encephalopathy diagnosed requires a comprehensive approach to identify the underlying cause and assess the extent of brain dysfunction. The diagnostic process often starts with a thorough physical examination to evaluate neurological function and detect signs indicative of metabolic encephalopathy. This initial assessment is crucial for determining the next steps in the diagnostic journey.
Advanced imaging techniques, such as magnetic resonance imaging (MRI), are used to identify structural abnormalities in the brain that may contribute to the condition. Electroencephalography (EEG) is recommended to rule out non-convulsive seizures, which can present similarly to severe acute encephalopathy. These tools provide valuable insights into the brain’s activity and help in making an accurate diagnosis.
Cerebrospinal fluid (CSF) analysis, obtained through a lumbar puncture, is another essential diagnostic tool. This procedure helps identify infections and inflammatory conditions affecting the central nervous system. Combined with other diagnostic methods, CSF analysis can provide a comprehensive picture of the patient’s neurological health, aiding in the effective treatment of metabolic encephalopathy.
Treatment Options for Drug-induced Metabolic Encephalopathy
Treating drug-induced metabolic encephalopathy treated involves addressing the root cause of the condition. This may include interventions like dialysis for uremic encephalopathy or the use of lactulose and rifaximin to reduce ammonia levels in hepatic encephalopathy.
Immediate and effective treatment is essential to prevent complications and improve patient outcomes.
Managing Acute Metabolic Derangements
Managing acute metabolic derangements requires prompt medical attention to stabilize the patient’s condition. Immediate interventions may include administering vital nutrients or fluids to address deficiencies. Adequate oxygen supply is also critical in managing acute metabolic encephalopathy.
In more severe cases, interventions such as dialysis may be necessary to treat metabolic encephalopathies like uremic encephalopathy. These procedures help stabilize the patient’s condition by removing toxic metabolites from the body and preventing further complications.
The urgency of treating acute metabolic derangements cannot be overstated. Timely medical intervention can prevent severe complications such as permanent brain damage, electrolyte abnormalities, and improve the overall prognosis for patients with metabolic encephalopathy.
Long-Term Management and Prevention
Long-term management and prevention of metabolic encephalopathy involve a combination of lifestyle changes and medical interventions. Preventive measures can include:
- Maintaining a healthy lifestyle with balanced nutrition
- Ensuring proper hydration
- Engaging in regular exercise to enhance overall brain health
- Promoting cognitive engagement
- Increasing physical activity to prevent complications
A tailored treatment plan is essential for managing symptoms effectively. This approach may include both pharmacological and non-pharmacological therapies. Many patients can experience a full return to normal mental function if treated promptly, although some may require ongoing support due to brain damage.
Preventing metabolic encephalopathy involves addressing both the condition itself and the underlying condition health issues that contribute to its development. By focusing on overall health and well-being, patients can reduce the risk of recurrence and improve their long-term prognosis to treat metabolic encephalopathy.
Complications and Prognosis
Metabolic encephalopathy can lead to severe complications if not treated promptly. One of the most significant risks is permanent brain damage, which can result in long-term cognitive deficits and impaired quality of life. Untreated metabolic encephalopathy can also lead to life-threatening complications such as coma.
Immediate medical intervention is crucial to prevent severe outcomes in patients with metabolic encephalopathy. Key points include:
- Patients require urgent medical attention to stabilize their condition and prevent lasting damage.
- Early diagnosis and treatment can significantly improve the prognosis.
- Early treatment reduces the risk of permanent complications.
For those who suffer permanent brain damage or acquired brain injury, ongoing support and therapy may be necessary to manage their condition effectively. This highlights the importance of comprehensive care and the need for continued medical and therapeutic support to improve patient outcomes.
Special Considerations for Critically Ill Patients
Critically ill patients with metabolic encephalopathy face unique challenges due to the rapid development of their acute state. These hospitalized patients often require admission to the intensive care unit (ICU) for close monitoring and specialized care. The hospital setting provides the necessary resources and expertise to manage severe cases effectively.
One of the challenges in treating critically ill patients is the potential for drug-induced encephalopathy. For example, cefepime-related neurological symptoms can develop days after starting the medication, emphasizing the importance of monitoring mental status in patients on this antibiotic. This requires healthcare providers to be vigilant and responsive to any changes in the patient’s condition.
Managing metabolic encephalopathy in critically ill patients involves a multidisciplinary approach. This includes addressing the underlying systemic illness, managing acute metabolic derangements, and providing supportive care to stabilize the patient’s condition. Early intervention and continuous monitoring are key to improving outcomes for these vulnerable patients.
Case Studies and Real-World Examples
A compelling case study involves a 52-year-old woman who developed encephalopathy after being treated with cefepime for sepsis. This case highlights the potential for antibiotic-induced neurotoxicity, especially in patients with compromised renal function. The patient’s encephalopathy symptoms, including altered mental status and clonic movements, were initially attributed to missed hemodialysis.
Once cefepime was discontinued, the patient showed significant improvement in her mental state, confirming the drug as the likely cause of her encephalopathy. This case underscores the importance of considering drug-induced encephalopathy in patients exhibiting neurological changes, particularly when renal function is compromised.
Approximately 3% of patients taking cefepime may develop encephalopathy, illustrating the need for healthcare providers to be aware of this risk and to monitor patients closely. Real-world examples like this case study provide valuable insights into the complexities of diagnosing and treating metabolic encephalopathy in clinical practice.
Summary
In summary, drug-induced metabolic encephalopathy is a complex and potentially life-threatening condition that requires prompt diagnosis and treatment. Understanding the various types of metabolic encephalopathy, their symptoms, and underlying causes is crucial for effective management. Early intervention can prevent severe complications and improve patient outcomes.
Healthcare providers must be vigilant in monitoring patients for signs of metabolic encephalopathy, particularly those with underlying health risks or who are critically ill. Real-world case studies highlight the importance of considering drug-induced causes and the need for a multidisciplinary approach to treatment.
In conclusion, staying informed and proactive in managing metabolic encephalopathy can make a significant difference in patient care. By recognizing the signs early and addressing the underlying causes, we can improve the quality of life for those affected by this challenging condition.
Frequently Asked Questions
What is metabolic encephalopathy?
Metabolic encephalopathy is a brain dysfunction resulting from metabolic disturbances, such as nutrient deficiencies or organ failure, which can manifest as cognitive and physical symptoms. Prompt identification and management of the underlying causes are crucial for recovery.
What are the common symptoms of metabolic encephalopathy?
Common symptoms of metabolic encephalopathy include confusion, disorientation, memory issues, and hallucinations. In severe cases, it may lead to loss of consciousness or coma. Recognizing these signs early is crucial for effective management.
How is metabolic encephalopathy diagnosed?
Metabolic encephalopathy is diagnosed through a comprehensive physical examination, along with advanced imaging techniques such as MRI, EEG, and analysis of cerebrospinal fluid obtained via lumbar puncture. This multifaceted approach helps ensure an accurate diagnosis.
What are the treatment options for drug-induced metabolic encephalopathy?
The primary treatment for drug-induced metabolic encephalopathy involves addressing the underlying cause, such as using dialysis for uremic encephalopathy or administering lactulose and rifaximin to lower ammonia levels in cases of hepatic encephalopathy.
What are the long-term management and prevention strategies for metabolic encephalopathy?
Effective long-term management of metabolic encephalopathy involves implementing lifestyle changes like balanced nutrition, hydration, regular exercise, and cognitive engagement, coupled with a personalized treatment plan that includes both pharmacological and non-pharmacological therapies. Prioritizing these strategies can significantly enhance outcomes and prevent recurrence.
